Latest Update
 27 Apr 2023
27 Apr 2023 The Effects of Sugar on Your Child’s Teeth
If you happen to be one of those who love sugary food items more than anything else, food items like cookies, pies, and ice cream form an important part of your food habit- then this article is for you! Did you know that there is sugar hidden in unsuspected food items like ketchup, fruit-flavored yogurt, spaghetti sauce, granola bars, and canned soup? It is easy for parents to restrict the sugar intake of their children when it comes to desserts, candies, and cakes, but when the sugar is disguised and hidden in seemingly healthy or harmless food, planning snacks and meals can seem to become slightly more complicated and overwhelming.
Kids usually tend to prefer both sweeter and saltier tastes as compared to adults and don’t have to learn to like sugar, because it’s actually a preference that’s biologically ingrained. Studies and research works conducted in recent times have proven that the body of a child might prompt more sugar cravings during their growth years, and their desire for sugar or sugary food items skyrocket during growth spurts when they need more energy and calories.
The American Heart Association states that children between 2 to 18 years old should not consume sugar more than 25 grams, of every day. Consuming sugar or sugary food items more than the stipulated amount can have a negative impact on the oral and overall health of your child.
In this article, we will try to narrate and articulate the impact of sugar on your child’s teeth and oral health, how to look for hidden sugar in food items and snackable, and present you with healthier alternatives to sugary food items.
If you have happened to notice that your child has developed dental cavities, or has developed more cavities than you think are appropriate, or his gums are red and swollen, get in touch with your child’s dental health expert or dentist, as soon as possible to schedule a regular thorough dental cleaning and examination.
Sugar vs. Teeth
There are at least billions of bacteria in our mouths. Proper oral hygiene habits, a healthy diet, and regular dental cleanings can keep the bad bacteria at bay and prevent them from overpowering the healthy bacteria.
When a person, young or old, consumes sugar, the harmful bacteria present in your mouth break the sugar to turn it into acid, which in turn leads to the softening of the enamel, eventually eating it away. As the harmful enamel bacteria spreads, outnumbers, and overpowers the healthy pH in your saliva, the mouth becomes more prone and susceptible to periodontal or gum diseases and cavities.
Sugar vs. Body
Besides causing oral health issues, consumption of way too much sugar can also be directly associated with childhood obesity and malnutrition. Consumption of sugar in unhealthy amounts can also lead to diabetes, a weakened immune system, and sluggish behaviors or lack of energy. Sugar can also be held responsible for brain fog, which can make focusing in school more difficult for children.
Sugar in Disguise
Remember that line from Romeo and Juliet? “What’s in a name? That which we call a rose by any other name would smell as sweet. “
This statement to universal in nature that it can also be applied to the domain of food items, especially sugar. It doesn’t matter what we call it, sugar will always have the same effect.
If you wish to look for the hidden sugar content in your food, look out for the names of the food labels, given below:
- High fructose corn syrup
- Rice syrup
- Any other kind of syrup
- Agave nectar
- Honey
- Fruit juice concentrate
- Evaporated can juice
- 100% fruit juice
- The suffix “-ose” (fructose, sucrose, dextrose, lactose, maltose, glucose)
Another way to watch out for hidden sugars is by checking the “added sugar” line on the food label.
Healthy Alternatives
Embarking on a new food journey can sometimes be confusing, let alone overwhelming. Allow us to help you lessen your stress and suggest doable suggestions to bring down the sugar intake of your child strategically. We have drafted a list of delicious, healthy, and low-sugar snacks that you can give to your child-
- Celery and cream cheese
- String cheese
- Popcorn
- Pretzels
- Guacamole and pita wedges
- Hard-boiled eggs
- Zucchini chips
- Parmesan fries
- Sweet potato chips
- Pepper nachos
- Besides these, there are other ways to restrict the sugar intake of your child. That includes:
- Limiting juice and soft drinks – choose water over every other drink and beverage!
- Keeping candy out of the home
- Only making desserts on special occasions
Protecting Your Child’s Smile
Practicing good oral hygiene and dental care regimen is important for everyone. However, for children who tend to intake sugar in larger quantities from their food items and drinks, cleaning their teeth thoroughly and effectively becomes even more significant and crucial.
If you are suspicious that your little one might be at risk of developing dental cavities because of the amount of sugar they are consuming, here are some suggestions to help protect their precious pearls and keep their smile from dental cavities and decay with or without cutting down on their sugary treats.
Use Fluoride
According to the American Dental Association (ADA), fluoride is a natural mineral that not only prevents tooth decay but can also reverse it in its initial days. it’s usually added to community water tanks or systems, as well as most kinds of toothpaste, so you have to ensure that your child is drinking plenty of fluoridated water and brushing their teeth at least twice regularly with fluoridated toothpaste. Dentists also recommend and provide professional fluoride treatments. Routine fluoride use has significantly brought down the number of children affected by dental decay.
Brushing Regularly
The most effective way to get rid of plaque from the teeth is by brushing regularly and effectively. Using the necessary amount of fluoridated toothpaste for their age, teach your child how to brush for the best results – brushing back and forth along the front, back, and top of the teeth, for at least two minutes, at least twice a day. The same bacteria that stick to the teeth also attaches itself to the surface of the tongue, so don’t forget to have your little one clean their tongue, too, to clean the bacteria that can lead to bad breath and other dental health and hygiene issues.
Flossing
Plaque doesn’t discriminate – not only does it wage wars on the visible surfaces of the teeth; but it also gets collected in between them. By showing your child floss daily, you’ll be enabling him and teaching them to break up all that plaque and get rid of it before it can lead to dental cavities and even eventual gum or periodontal diseases.
Drink More Water
Water is the best thing your child can possibly drink! Not only does it keep them hydrated, but it’s good for their body and also works wonders for their dental health. Since almost all kinds of tap water contain fluoride, ensuring that your child drinks water after consuming sugary or acidic foods helps dilute and rinse away any cavity-producing bacteria in between brushings. Water is also functional in producing saliva in abundance, which acts as a natural defense mechanism against plaque acids.
Visit a Children’s Dental Health Expert
One of the best ways to fight tooth decay is to visit a dental health expert at regular intervals.Your child’s first dental appointment should be scheduled as soon as the first tooth sprouts out. He or she should visit the dental health expert for regular thorough cleaning and examination sessions, once every six months or twice a year.
 27 Apr 2023
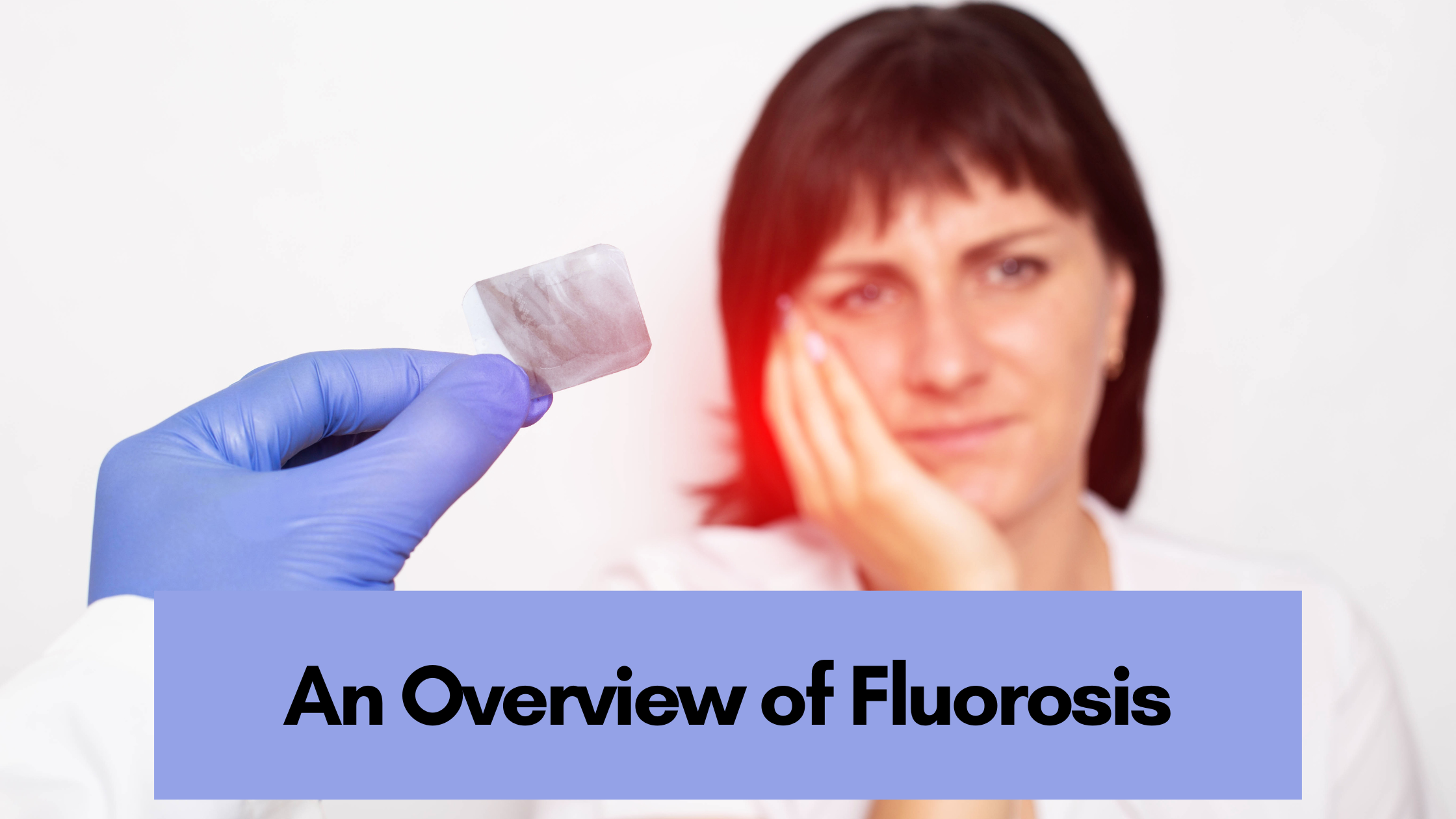
27 Apr 2023 An Overview of Fluorosis
Fluorosis is a condition that leads to the formation of white or brown stains on your teeth. Overexposure to fluoride in the initial years of life when your permanent teeth are developing- is one of the primary reasons behind it. Fluorosis is a cosmetic concern – definitely not a medical concern and will not have adverse effects on your health. But there are treatments, however, that can take care of the issue.
What Is Fluorosis?
Fluorosis is a cosmetic dental concern that’s understood by the formation of white or brown spots or stains on the surface of your teeth. These stains or spots usually vary from tiny white flecks that are nearly visible to dark brown blotches that are clearly visible.
Whom Does Fluorosis Affect?
Dental Fluorosis affects people who were primarily overexposed to fluoride during their developmental years before their adult or permanent teeth show up completely. Children below the age of 8 years are more susceptible to developing fluorosis. Teeth that have already sprouted can’t be affected by fluorosis.
How Common Is Fluorosis?
Mild fluorosis is absolutely common, affecting almost 1 out of every 4 Americans between the ages of 6 to 49. Moderate to severe Fluorosis is comparatively less widespread in the U.S.
Does Fluorosis Weaken Teeth?
No, dental fluorosis has nothing to do with oral health or function. People with fluorosis are actually more immune to cavities. This surprising fact is what led health officials to introduce fluoride into public water supplies at medically safe levels. This simply means that the water supply systems have sufficient fluoride to help prevent tooth decay, but not enough to lead to fluorosis. The Centers for Disease Control and Prevention (CDC) recommends the usage of 0.7 milligrams of fluoride per liter of water is the recommended level.)
What Are the Symptoms of Fluorosis?
Dental discoloration is the only tell-tale symptom of fluorosis. The extent of discoloration is dependent on the severity of the condition. Dentists usually use the following terminologies to categorize fluorosis:
- Questionable: A few very light white flecks and white spots.
- Very mild: Light white areas covering less than 25% of your tooth surfaces.
- Mild: Light white areas covering less than 50% of your tooth surfaces.
- Moderate: White or light brown areas covering more than 50% of your tooth surfaces.
- Severe: White, light brown, or dark brown spots affecting all surfaces. Your teeth may also have pitting (small depressions in your tooth enamel).
In some of the milder cases, the dental discoloration can be so light that it can even evade the scrutiny of the dentist. But if fluorosis seems to have a negative impact on your self-esteem, cosmetic dental treatments can be a way to go.
What Are the Reasons for Fluorosis?
Dental fluorosis takes shape when a child is consistently ingesting or is experiencing way too much exposure to fluoride in some way or the other, while their permanent teeth is still developing underneath their gums. This can often stem from drinking heavily fluoridated water or swallowing fluoridated toothpaste while brushing their teeth.
Dental fluorosis in adults is not a usual phenomenon. It only affects people who are still developing their permanent or adult teeth.
How Is Fluorosis Diagnosed?
Your dentist can diagnose fluorosis during a routine dental examination.
Does Fluorosis Go Away?
Fluorosis is usually there to stay and doesn’t go away with brushing or flossing. The only available way to take care of it is with the help of cosmetic dental treatments like dental bonding, veneers, and crowns. These treatments are discussed in the following sections.
How Do You Get Rid of Fluorosis?
There are available cosmetic dental procedures that can take care of fluorosis. The treatment that’s suitable for you is dependent on multiple factors, including the severity of fluorosis, your budget, and your own personal choices. Common fluorosis treatments include:
Teeth Whitening.
A bleaching gel is applied to your teeth for a stipulated amount of time. The gel is used to lighten the enamel of your tooth, so the stain blends with the original color of your teeth. While teeth blending is the way to go for milder cases of fluorosis, other treatments might be good for you.
Dental Bonding.
A tooth-colored composite resin is used to cover up fluorosis to hide the stains, for this procedure. Your teeth are then shaped and polished to make them resemble the natural ones.
Dental veneers.
Composed of resin or porcelain, veneers are thin shell-like structures that adhere to the frontal surfaces of the teeth. Veneers are usually personalized, so your dentist is going to need your dental impression to get the size and fit right.
Dental Crowns.
Like veneers, crowns too are personalized. Having said that, dental restoration of this category fits over your entire tooth. Your dental health expert will require to remove some of the natural enamel so the crown sits appropriately.
Enamel Microabrasion.
This is a process too; your dental health expert will need to take a small section of the enamel of your teeth. This helps in the elimination of some of the fluorosis stains. The dentist sometimes will then follow microabrasion with teeth whitening to get a uniform color on your teeth.
How Can I Reduce My Child’s Risk for Fluorosis?
To bring down your little one’s risk for fluorosis, be careful about the amount of fluoride they are exposed to.Find out about water fluoridation laws in your area, or test your well water for fluoride levels. You might not want your child to be overexposed to fluoride , however, they also need an appropriate amount of fluoride as they grow and develop. Thus, the proper amount of fluoride is significant for the growth and development of your child’s oral health conditions and dental hygiene.
In addition, you should:
Make sure your child spits toothpaste out instead of swallowing it.
Limit your child’s consumption of sugary and acidic foods and beverages.
Practice good dental hygiene habits with your child.
Visit your dentist at least every six months for routine dental check-ups.
What’s The Outlook for People with Fluorosis?
Fluorosis has no adverse effects on your dental or overall health whatsoever. From a medical point of view, you don’t require any medical attention for this if you don’t want to. However, if your condition is embarrassing you or is hampering your self-esteem, cosmetic dentistry can help you get back your precious and confident smile dramatically.
When Should I See My Healthcare Provider?
As we have already discussed, you don’t need any additional medical attention if you are not self-conscious or embarrassed about it. Your dental health expert will discuss and consult your treatment plan with you before proceeding.
 27 Apr 2023
27 Apr 2023 Is Chewing Gum Good for Your Teeth?
Chewing gums have them there for centuries now, but not all chewing gums have been created equally- “equally”, in every connotation of the term. They are usually sold with candies and lozenges on the shelves, with sugary chewing gums, but not all chewing gums are harmful to the teeth. Some of the chewing gums have legitimate benefits for your oral health and dental hygiene. In this article, we will try to learn more about the benefits of chewing gum on your oral health.
What Is the Best Chewing Gum for Your Teeth?
The Oral Health Foundation suggests that chewing sugar-free gum stimulates the production of saliva, which helps rinse away the leftover food particles, rinse away the harmful bacteria, strengthen teeth, and reduce the amount of acid in your mouth that is responsible for eating away the enamel of your tooth. Some chewing gums have benefits, often more than one. The benefits include:
- Prevent cavities
- Strengthen enamel
- Increases saliva flow
Gum Ingredient Xylitol Is Good for Your Teeth
Chewing gums have been proven to be effective in preventing the formation of cavities if it contains a natural sweetening agent called Xylitol. Xylitol is a kind of sweetener that occurs naturally and has been proven to bring down the amount of dental cavity-causing bacteria in plaque. This observation was a result of multiple research studies in the year 2017. Xylitol is also known to enable the neutralization of the acids produced by the bacteria, keeping the dental enamel stronger. Another significant additional leverage in the fight against tooth decay.
Can I Strengthen My Teeth by Chewing Gum?
Some of the brands of chewing gums have an added substance called casein phosphopeptide-amorphous calcium phosphate (CPP-ACP). CPP-ACP, also popularly called Recaldent. This chemical substance is known to remineralize or slow down tooth decay. It is advisable for people who struggle with an allergy to milk and milk products to not use products that contain CPP-ACP.
How Often to Chew Gum?
Hold your horses before you get too carried away about chewing gums. There is an appropriate time and place to chew it, in a way that will benefit you’re your dental health conditions and oral hygiene. To achieve the best possible results, chew the gum after your meal or drink water, which will also help to rinse away the leftover food particles and sugar from your teeth and gums.
Chewing too much gum can lead you to experience jaw pain. Should this happen, it is your cue to cut back, Studies have also found a direct association between chewing gum and TMJ or Temporomandibular Joint disorders, especially among teenagers and younger adults. Temporomandibular Joint (TMJ) disorders are medical conditions known to adversely affect the jaw joints and the surrounding ligaments and muscles. It can usually be caused by trauma, an improper bite, arthritis, or general wear and tear. The common tell-tale signs and symptoms of TMJ include jaw tenderness, headaches, earaches, and facial pain. Moreover, certain sugarless sweeteners more often than not, are responsible for an upset stomach if consumed in abundance.
What Gum Should I Chew?
When you are about to purchase chewing gums from a random grocery or convenience store, look for sugarless chewing gums that have the ADA seal on the package. The ADA seal ensures that the product is safe for consumption and is beneficial product for oral health and dental hygiene.
There is a huge selection of chewing gums including sugary and sweet candies, available in the market. But it is always wise to read the ingredients thoroughly before reaching out for the most indulgent one on the shelves, which can also harm your teeth. Choose the ones that have ingredients that can fight plaque and dental decay. Your future self and your teeth will thank you.
3 Tips for Choosing a Tooth-friendly Gum
1. Choose a Saliva-Stimulating Flavor
Some chewing gum flavors stimulate comparatively more production of saliva than others. Several scientific studies have brought out that strawberry-flavored gum stimulates the most amount of saliva production, especially during the first minute of chewing. Watermelon- and apple-flavored gums too enhance the production of saliva almost as much as strawberry-flavored gum.
If you happen to prefer the conventional mint or cinnamon-flavored gums, then you need to know that these chewing gums have not been proven to stimulate saliva production not as much as the fruity flavors. However, spearmint and cinnamon-flavored gums are comparatively more effective at bringing down the acidity of your mouth than the ones with fruity flavors.
2. Avoid Gum that Contains Citric Acid
Certain sugar-free chewing gums, especially the ones with sour flavors, contain citric acid. Chewing gum that citric acid can acidity in your mouth as a whole when you chew it. Cavity-inducing bacteria thrive in an acidic environment. Chewing gums containing citric acid can also cause the dental enamel to erode, especially when chewed more frequently than is appropriate. Erosion caused by the acid inside the mouth is a form of chemical wear and tear on the dental enamel and cannot be reversed.
Check the packaging of the sugar-free gum to make sure that it does not contain citric acid and to ensure your gum improves your oral health instead of wreaking havoc on it.
3. Look for Sugar Substitutes that Kill Bacteria
Sugar-free gums use various other sugar substitutes to flavor the chewing gum. Many of them are sweetened with sorbitol and/or maltitol, which are sugar substitutes that are known to not enhance the process of tooth decay. While these sugar substitutes are not bad for your oral health, chewing gums that contain xylitol or erythritol have added dental health benefits comparatively more than those offered by gums containing more common sugar substitutes.
If you happen to chew gums that are sweetened with xylitol, cavity-causing oral bacteria consume the xylitol like they would consume sugar, which is their primary source of food. However, xylitol is fatal for these bacteria and they die instead of growing powerful.
Surprisingly, xylitol only kills the bad, cavity-causing bacteria in your mouth and it does not affect the healthy bacteria. Consuming xylitol might also be beneficial to your body to absorb more of the calcium your intake which can help strengthen your teeth as a whole.
If you don’t seem to find a sugar-free gum that contains xylitol at your disposal, then try a gum sweetened with erythritol. Erythritol, like Xylitol is known to obliterate the cavity-causing bacteria in your mouth to further prevent dental decay or cavities.
If you struggle with the frequent development of cavities, then it is advisable that you chew gums several times a day. You might notice that there is a magical drop in the frequency of the development of cavities.
 22 Apr 2023
22 Apr 2023 Braces Care Instructions
Dental braces tend to trap a lot of food particles against the gums and teeth. That is exactly why you should carefully understand and follow the braces care instructions from your orthodontists. You are required to follow these rules and regulations to maintain a healthy smile during the span of the treatment.
Through this article, we will discuss how to brush and floss your teeth while you have your traditional metal braces on. we will also discuss what food to steer clear of and how you can deal with minor orthodontic inconveniences at home, with ease.
Brush Your Teeth After Every Meal
It is very important that you brush your teeth at least twice every day. We would also recommend that you brush your teeth 30 minutes after every meal if you have braces on. The waiting period of 30 mins is important for your saliva to wash all the acids from your food.
Brush your teeth like this:
- Brush the outside of each tooth.
- Brush where your gums and teeth meet using a circular motion.
- Brush the inside surface of each tooth.
- Brush the chewing surfaces of your teeth.
Floss Once a Day
The best place for the plaque to hide is the unreachable places between your teeth and gum. That makes flossing every day, at least once very important for your hygiene. A floss threader is easily available at your nearest pharmacy and helps you floss with your braces on.
Floss your teeth like this:
- Thread floss through the threader and slip it up behind your archwire.
- Pull the floss between two teeth and up under your gum margins.
- Rinse with clean water.
Strengthen Enamel with Fluoride
Use fluoride-based toothpaste and fluoride-based mouthwash. Fluoride helps strengthen the enamel of your tooth and significantly brings down the risk of dental cavities.
Avoid Sticky, Hard-to-Chew Foods
You can eat almost all of your favorite foods with your metal braces on. However, there are a few food items that you should try to avoid to not encounter any inconveniences.
Please Stay Away from These Troublemakers:
- Sticky chewy foods like taffy, caramels, and jerky
- Hard foods like raw carrots and apples, unless cut into bite-size pieces
- Crunchy foods like corn chips, popcorn, almonds, and corn nuts
- Candy and other sweets, unless in moderation
- Sugary beverages like fruit juice, sports drinks, and pop
Take Care of Poking Wires or Brackets
You need to get your poking wires or loose brackets fixed from time to time, during your visits to the dentist’s office. However, there are many minor and insignificant issues that you can easily take care of at home.
- If your wires start poking, trim the wire with clean nail clippers.
- If a bracket is irritating your cheeks, place a small piece of braces wax on the offending bracket.
- If a bracket comes loose, your dentist is most likely to replace it during your next visit.
Maintain a Healthy Oral Hygiene Routine
Take a moment to check and rearrange your dental health and oral hygiene practices to rate yourself higher on the oral hygiene spectrum. Your aim should only be to prevent any permanent or irreversible damage to your gums and teeth, for the sake of your precious smile.
 22 Apr 2023
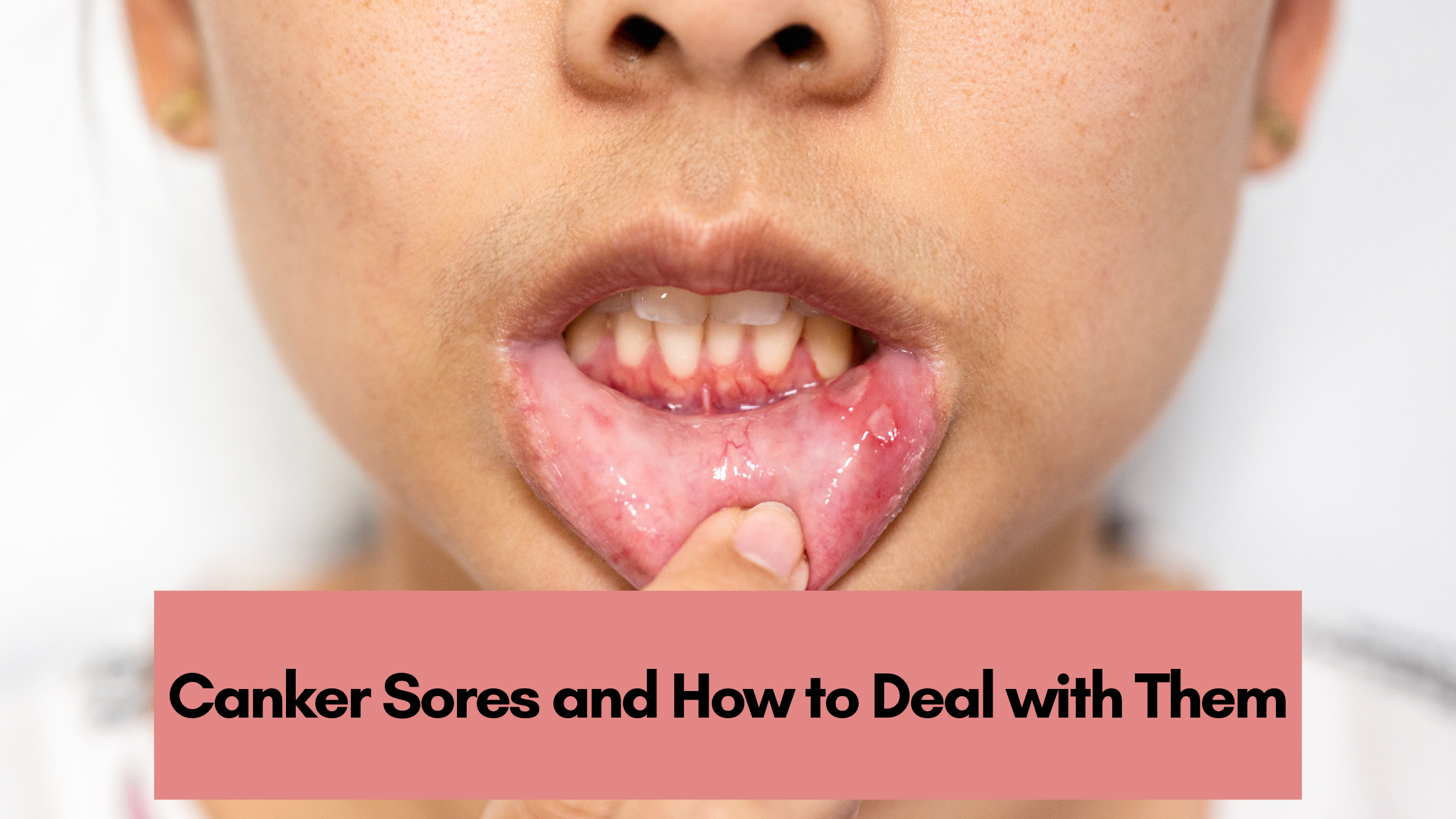
22 Apr 2023 Canker Sores and How to Deal with Them
What Are Canker Sores?
An aphthous ulcer or a canker sore is usually a painful and open mouth ulcer or sore. It is the most common type of mouth lesion.
Certain people often happen to notice them on the inside of their cheeks or lips. They are usually surrounded by red, inflamed soft tissue – filled with white or yellow pus.
The symptoms of canker sores include:
- A small white or yellow oval-shaped ulcer in your mouth
- A painful red area in your mouth
- A tingling sensation in your mouth
In some cases, other symptoms might also be present, including:
- Swollen lymph nodes
- A fever
- Not feeling well
Canker sores are not known to be contagious. They naturally heal or get better within a span of 1 to 3 weeks, and the pain usually subsides within 7 to 10 days. However, serious canker sores might even take up to 6 weeks to subside or get better.
How to Treat a Canker Sore?
Canker sores can usually eventually heal with additional medical attention. Besides that, there are multiple beneficial lifestyle changes that you can adhere to treat the lesion caused by a canker sore.
The first and the most basic habit, for instance, is to thoroughly brush and floss your teeth twice every day to prevent any bacterial infection and to maintain a proper dental health and oral hygiene regimen. It is also advisable that you try to avoid spicy food to avoid unnecessary pain and trouble and to speed up the healing process.
Pain might often get out of hand. You can try to subside and lessen the discomfort by gargling with mouthwash or lukewarm saltwater. It might possibly get a tad bit uncomfortable at first, will help you seek relief from the pain.
Some of the over-the-counter medications or topical products can enable the process of healing the canker sores and providing relief. These medications or topical products include:
- Benzocaine (Orabase, Zilactin-B, Kank-A)
- Hydrogen peroxide rinses (Peroxyl, Orajel)
- Fluocinonide (Vanos)
Your general physician or dental health expert might also prescribe:
An antibacterial or antimicrobial mouth-washing liquid, such as Listerine or other mouth-washing liquids includes chlorhexidine (Peridex, Periogard) and hydrogen peroxide.
Antibiotic drugs like mouthwashes or pills that contain doxycycline (Monodox, Adoxa, Vibramycin). They are prescribed usually for recurrent, or returning, canker sores.
A corticosteroid ointment, such as hydrocortisone hemi succinate or beclomethasone
Topical anesthetics, such as benzocaine.
A medically prescribed mouthwash, especially the types that contain dexamethasone or lidocaine for healing inflammation and subside the pain
There are primarily two main types of canker sores:
Simple Canker Sores.
These might appear and reappear three or four times every year and stay up to a week.
Complex Canker Sores.
These are comparatively uncommon kinds and tend to occur more often in people who have previously had them or have a family history.
Are Canker Sores An STI?
No, canker sores are not like herpes or any other type of sexually transmitted infection or STI. Truth be told, they are not even communicable or contagious. So, the good news is you cannot spread or catch them through kissing or any form of sexual contact.
Who Gets Canker Sores?
Anybody, under the sun, can develop canker sores. But they are commonly seen among teenagers, young adults, or people in their 20s. Women and people assigned female by birth (AFAB) are more susceptible to getting canker sores as compared to men and people assigned male by birth (AMAB). Medical experts seem to believe that it could possibly be because of hormonal changes.
How Common Is This Condition?
Canker sores are fairly common among people as we have already discussed. About 20% of the population in the U.S. have experienced canker sores at least once in their lifetime.
Symptoms
Canker sores can manifest through several symptoms, which might vary based on the type of lesion.
Minor Canker Sores
Minor or less severe canker sores and lesions are some of the most common types of canker sores. Having said that, they might be painful in nature, but they subside and usually heal on their own without any additional medical attention and without leaving any marks behind around 1 to two weeks after their appearance.
- Some of the most common and prominent symptoms that can be directly linked with minor canker sores include:
- Small, oval-shaped bumps inside the mouth
- A tingling or burning sensation
- Pain when eating, drinking, or speaking
Major Canker Sores
Major canker sores are less common than minor canker sores and can also cause more severe symptoms. They can take up to 4 weeks to heal and may cause scarring.
Symptoms of major canker sores include:
- Large, round bumps or swellings inside the mouth
- Tingling, burning, or inflammation with visible redness
- Severe pain or discomfort
- Difficulty eating, drinking, or speaking
Herpetiform Canker Sores
Herpetiform canker sores are very rare and uncommon. Among the very few people who develop canker sores in general, only about 5% of them struggle with this type of lesion.
In the rarest of rare cases, they can merge together and form a cluster-like situation. Should this occur, it can easily take up to several weeks to subside and heal, and might also heighten the possibility of leaving a scar behind.
There are some possible tell-tale signs of herpetiform canker sores. These signs and symptoms include:
Small, pinhead-sized bumps inside the mouth, could shape up form in clusters
Tingling or burning in the mouth or general discomfort
Pain, which may be worse when chewing, drinking, or talking
Home Remedies for Canker Sores
Applying ice or tiny amounts of milk of magnesia to your sores can help relieve pain, and promote and speed up the healing process.
Rinsing your mouth with a mixture of warm water and baking soda (1 teaspoon per 1/2 cup of water) can also help with the pain to subside and heal.
Honey has been scientifically proven to be effective in treating canker sores as well.
Causes And Risk Factors
Your risk of developing canker sores increases if you happen to have a family history of these lesions. Canker sores are known to have umpteen reasons and causes to develop; however, the most common ones include:
- Viral infection
- Stress
- Hormonal fluctuation
- Food allergy
- Menstrual cycle
- Vitamin or mineral deficiency
- Immune system problem
- Mouth injury or trauma
- Acidic foods, such as citrus fruits.
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen.
- Dental appliances, such as braces or ill-fitting dentures.
A deficiency in certain vitamins, including categories like B3 or niacin, B9 or folic acid, and B12 or cobalamin, can lead you to get canker sores. Zinc, iron, or calcium deficiencies can also trigger, enhance and worsen canker sores.
In some of the cases, the original cause of a canker sore could not the effectively determined.
Complex canker sores may develop in people with immune system conditions, including:
Lupus.
Behcet’s disease.
Celiac disease.
Ulcerative colitis.
Crohn’s disease.
AIDS.
Canker Sores Vs. Cold Sores
There are certain noticeable similarities between cold sores and canker sores as well. However, as opposed to cancer sores, cold sores can ever appear on the outside of your mouth i.e., your face. Cold sores can even tend to appear as blisters, not inflamed sores, and transition into being sores after the blisters pop open.
The primary villains behind the causation of cold sores are the herpes simplex virus. This virus is pre-existent in your body and can be triggered by stress, exhaustion, and even sunburn. Cold sores can tend to appear on your lips, nose, and even your eyes.
How A Canker Sore Is Diagnosed?
Your doctor will have to examine the sore or lesion before reaching a conclusive diagnosis.
They may recommend some specific blood tests or happen to require a biopsy of the area if there is a visibly severe outbreak of the sores, or if they think that you might have a:
- Virus
- Vitamin or mineral deficiency
- Hormonal disorder or imbalance
- Problem with your immune system
- Severe breakout
A cancerous or malignant lesion, oftentimes might as a canker sore, but it is going to need urgent medical attention to heal and get better. Some of the signs and symptoms of oral cancer are similar to those of canker sores, including symptoms like painful and uncomfortable ulcers, and swelling in or around your neck.
But oral cancer can often be indicated and differentiated from canker sores by some unique tell-tale symptoms, including:
- Bleeding from your mouth or gums
- Loose or wobbly teeth
- Trouble swallowing
- Earaches
If you happen to experience any of these above-mentioned symptoms along with the ones for canker sores, seek for immediate medical attention to rule out oral cancer as a cause for all the additional inconveniences.
Complications Of Canker Sores
If your canker sore doesn’t seem to subside, heal or resolve in a few weeks span, you might have to go through some more serious consequences and complications. These complications might include:
- Discomfort or pain while talking, brushing your teeth, or eating
- Fatigue, severe exhaustion, or physical sluggishness
- Sores spreading outside of your mouth
- Fever
- Cellulitis
- Lesions are unusually large.
- Last longer than two weeks.
See a doctor or a health care provider if your canker sore or lesion is causing excruciating pain or is interfering with your day-to-day activities concerning your mouth, and no home remedies and working as they should.
It is recommended that you do this even if the complications have developed within just 7 to 14 days of the appearance of the sores and lesions.
Microbial or bacterial infections can spread and can be followed by more serious issues or ailments, so it is crucial to control or stop a probable bacterial cause of a canker sore at the earliest.
Tips and Ways to Prevent Canker Sores
You can prevent the occasional recurrence of a canker sore outbreak by steering clear of those food items that might have previously triggered an outbreak. These often include food items that are salty, spicy, or acidic in nature. Also, it is recommended that you avoid food items that trigger allergy symptoms such as an itchy mouth, a swollen tongue, or hives.
If an appearance of a canker sore is triggered by stress, it is advisable that you try stress reduction methods and self-calming techniques, including meditation, deep breathing, or music therapy.
Practice a good oral health and dental hygiene regimen and use a toothbrush with soft bristles to save your gums and soft tissues from scratches and irritation.
Consult your healthcare provider to determine and understand if you have a specific kind of vitamin or mineral deficiency. They can assist you to draft a suitable diet plan and prescribe individual supplements if you happen to require them.
Contact your healthcare provider or dental health expert if you happen to develop:
- Large sores
- An outbreak of sores
- Excruciating pain
- A high fever
- Diarrhoea
- A rash
- A headache
- High fever and physical sluggishness
Seek immediate medical attention if you are unable to drink or eat or talk, or if your canker sore has not subsided or healed within 3 weeks.
To Conclude
Canker sores and lesions can be pretty inconvenient and painful to deal with and might be triggered by a large variety of factors. In most cases, canker sores eventually heal and subside on their own without any additional medical attention or treatment. There are also some time-tested and easy home remedies available to help them soothe and heal faster, along with multiple other ways to prevent them from appearing in the first place.
Having said that, it is always wise to get in touch with your healthcare expert if your canker sore has not subsided or healed even after a week or two, or if you happen to develop and experience comparatively more severe symptoms and complications.
Canker sores can be extremely irritating and uncomfortable, but usually not dangerous. As opposed to cold sores, canker sores are not caused by infections and cannot be spread or transmitted from person to person. Most people choose to use over-the-counter drugs to soothe and heal canker sores faster. But if you happen to not notice any visible improvement even after using those over-the-counter products, it is a cue for you to get in touch with your healthcare provider or a dental health expert. They can prescribe specific medicines to help you take care of them are getting back to normalcy without much hassle.
 19 Apr 2023
19 Apr 2023 Does Osteoporosis Affect Your Teeth?
Osteoporosis is a bone disease that leads to the loss of bone density and mass. It can also cause the bones to weaken, which skyrockets the risk of fractures in turn.
Like multiple people struggling with osteoporosis, you might want to know if it affects your teeth as people say. The simple answer to that is – not directly. Considering your teeth aren’t actually bones, osteoporosis itself cannot be influential in changing your dental health or composition.
Having said that, osteoporosis does have an indirect impact on your dental health. This is primarily because it can change the integrity of your jaw, which will affect how your teeth are held in place. Truth be told osteoporosis has been linked with heightened chances of tooth loss for a reason.
Only brushing your teeth doesn’t suffice when you are struggling with osteoporosis. It is also important that you know how osteoporosis might affect your dental health.
What Are Teeth Made Of?
Teeth and bones do share some common characteristics; however, they are not made of the exact same materials. Your bones are mainly made of collagen and the mineral calcium phosphate. Teeth, on the other hand, have the four following layers:
#1. Enamel is the hard calcified tissue on the top (crown) of teeth that isn’t made of living cells
#2. Cementum is another type of hard tissue that protects a tooth’s root
#3. Dentin is below enamel and cementum, making up most of our teeth’s interior and providing structure
#4. The pulp is the innermost layer of our teeth and contains nerves and blood vessels
Osteoporosis is known to damage the bones’ ability to produce new tissue to make up their spongy interior. People often tend to mistake teeth for bones because the whitish enamel covering the crown of your teeth looks like bone. Unlike your bones, however, the enamel isn’t made of living tissues.
Research Findings
The connection between osteoporosis and tooth loss is already out there and has been subjected to umpteen scientific research works. These include:
The Osteodent study in 2009 measured the bone density of a subject of 651 women. The researchers found that women with osteoporosis had the tendency to have three fewer teeth on average as compared to the women who didn’t have the condition.
Again, survey data was collected from 333 people, 27% of whom were struggling with osteoporosis. These scientists concluded that having osteoporosis was “significantly correlated with reduced tooth number,” specifically for molars.
Another recent study conducted in 2017 concluded that postmenopausal women in the South Indian region had a higher chance of experiencing tooth loss, should they develop osteoporosis.
Researchers were quite clear when they mentioned that osteoporosis and tooth loss are directly linked, but they are yet to find out the exact nature of the correlation.
.
A primary theory of the correlation that is as osteoporosis progresses, your jawbone weakens and loses its appropriate density. As the jawbone weakens, teeth begin to get unstable. The changes in the structure and the integrity of the jawbone also affect the alignment of the teeth, often damaging the roots of the teeth and causing oral complications.
Osteoporosis Medications and Teeth
If you happen to take medication for osteoporosis, it is advisable to consult with your health expert about the probable impact on the teeth. Medications that are used to strengthen the bones can negatively impact the teeth and jawbone, unfortunately.
The treatment usually prescribed to people struggling with osteoporosis is bisphosphonate therapy. Bisphosphonates, can help in the strengthening of bones and help prevent fractures, and can be orally or intravenously administered. Multiple people also intake calcium or vitamin D, with bisphosphonates, as advised by the American College of Rheumatology.
Truth be told bisphosphonates do pose a threat to your jaw and teeth. Treatments under this category can be directly connected to the development of a rare degenerative condition called osteonecrosis of the jaw (ONJ). The Endocrine Society warned about the risk of developing ONJ is the highest after dental surgery. The frequency of the occurrences in people who have undergone “high-dose, long-term therapy, as might be given during cancer treatment”, increases.
Keeping Bones and Teeth Healthy
One of the crucial things that you can put at the top of your priority list is the health of your bones and teeth by maintaining a healthy dental care and oral hygiene regimen that can add and benefit to your overall well-being.
#1. Some key factors include:
#2. Eating a balanced diet
#3. Making sure you get 600 to 800 iu of vitamin D each day
#4. Aiming for 1,000 to 1,200 milligrams of calcium each day
#5. Not smoking, or considering quitting smoking if you currently smoke
#6. Limiting your consumption of alcohol
#7. Being physically active — the world health organization (WHO) has exercise guidelines by age group
If you happen to be facing trouble in the intake of enough calcium or vitamin D from your diet, it is wise to mention it to your doctor or your nutritionist about taking a supplement. It is advisable that you take supplements only as directed or prescribed.
Maintaining proper dental health and oral hygiene regimen is an important part of the long-term health of your precious pearls. The ADA or American Dental Association (ADA) recommends the following:
- Brush your teeth thoroughly twice a day for 2 minutes per session.
- Use toothpaste containing fluoride when brushing your teeth.
- Clean between your teeth daily (including flossing, interdental brushes, and others).
- Limit your intake of sugary beverages and snacks.
- Aim to visit your dentist for regular check-ups.
If you are taking resorptive agents like bisphosphonates, mention it to your dentists so they can include it in your treatment plan, especially if you have or will be undergoing procedures like tooth extraction. If your dentist knows and is able to accommodate it in your plant properly, you will probably not have to stop taking the medicine and not skip the process- both ends can be saved.
Know Your Risk
Keeping a track of your oral health is necessary especially if you already have dental health issues or if you already have the risk factors of osteoporosis.
Your chances of getting osteoporosis heighten with age. Women are more likely to struggle with osteoporosis, and the loss of estrogen that is followed by menopause can also add to it.
Treating Osteoporosis
There is no current cure for osteoporosis, so prevention is the best way to go. However, there are multiple ways to manage osteoporosis and treatment options, according to research conducted in 2018 research.
Certain medicines for osteoporosis are meant to prevent bone loss, (also called antiresorptive medication), while others are meant to regrow the bones (also called anabolic medicines). Both categories of drugs are formulated to increase bone density and prevent bones from getting fractured in the future.
Based on your particular needs and health, your doctor might prescribe the following:
Bisphosphonate Medications.
These are usually the initially prescribed medicines for postmenopausal women, and they function by slowing the corrosion of the bones.
Selective Estrogen Receptor Modulators (SERMs).
This category of medication is also called estrogen agonists. SERMs are mostly raloxifene, used to treat osteoporosis in women, and also other serious conditions like breast cancer.
Hormone Replacement Therapy.
These medicines are the synthetic version of our natural hormones. The loss of estrogen owing to menopause can also add to osteoporosis, estrogen therapy might also prove beneficial, however, it is not the conventional first-line treatment of osteoporosis. Testosterone therapy functions similarly to treat estrogen in men.
Antibody Medications.
Popularly known as biologics, these can also slow down the process of bone erosion and catalyze the process of the formation of new bones. The two available drugs are denosumab and romosozumab, both administered through injections.
Parathyroid Hormone Therapies.
PTHs or Parathyroid Hormones are formulated to increase bone density and strength, helping the prevention of fractures and helping the healing process of old fractures. The PTH drugs teriparatide and abaloparatide are approved by the FDA and are usually administered through injections to treat osteoporosis.
Calcitonin.
It is an artificial version of a hormone that is secreted by your thyroid gland that regulates and controls calcium. It is approved by the Food and Drug Administration (FDA) and is administered in the form of nasal sprays. It is used for treating osteoporosis in certain premenopausal women.
Calcium and Vitamin D Supplements.
These are crucial in building and maintaining strong bones and teeth.
PT or Physical Therapy is also used to treat osteoporosis and aims to strengthen muscle and bone to save the patient from future fractures. A Pt regimen is usually personalized specifically to your needs. It can also be done in some minutes every day at home or at regular sessions with some assistance from your physical therapist.
Conclusion
Treatments for osteoporosis can bring down the progression of the disease and in certain cases enable bone growth and development. Your dental health expert can help you address your oral complications and conditions that might take place owing to osteoporosis or the associated treatment.
 19 Apr 2023
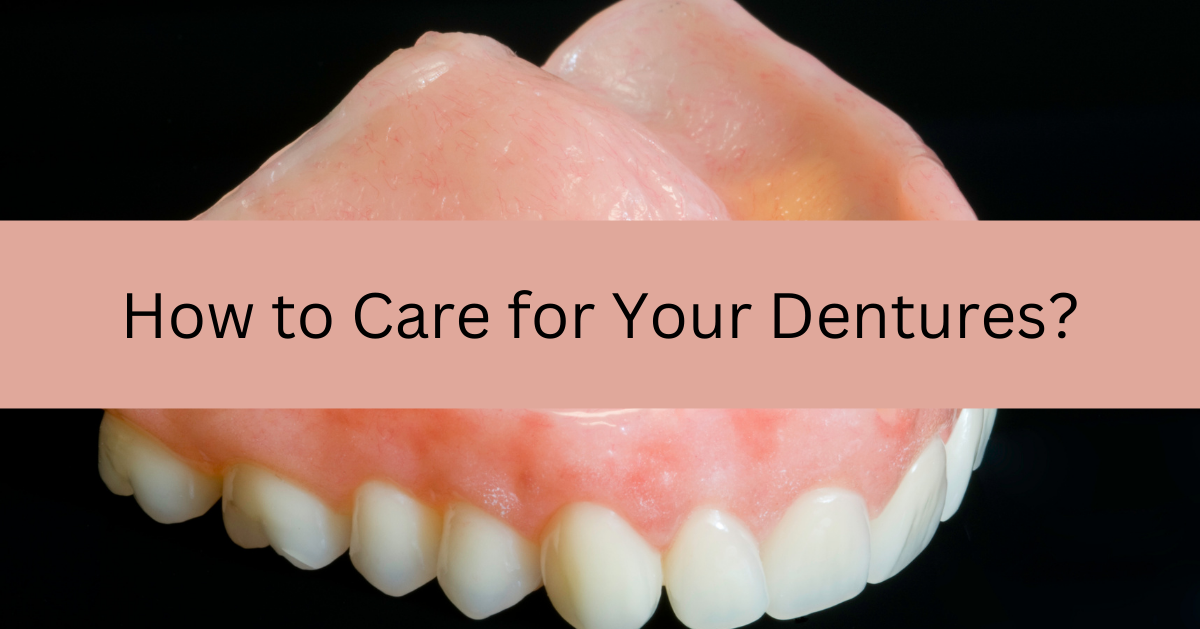
19 Apr 2023 How to Care for Your Dentures
Complete or partial dentures or removable teeth can be used as a replacement for the lost teeth, fixing the appearance of your face. These artificial teeth are made to resemble the natural ones and are made from an amalgamation of different materials like acrylic and metals. You have to clean them properly every day, irrespective of their originality. Cleaning your dentures includes more than just brushing though, there are other steps involved to keep them clean and maintain a good personal oral and dental hygiene regimen. Stay with us till the end to learn more!
What’s The Best Way to Clean Your Dentures?
Sticky food and plaque stick to dentures as they stick to the natural teeth. Dental plaque is a thin sticky film-like formation of bacteria that forms on the dentures and teeth after consuming food and drinks. If you don’t clean your dentures regularly and properly, you are allowing the plaque to build up, which will then be followed by gum diseases and bad breath. Cleaning your dentures and teeth regularly is important to maintain your overall oral and dental health. Given below is a list of a few things and suggestions that you might want to get to keep your dentures clean:
- A soft-bristled toothbrush
- Water
- Denture cleaning solution or mild soap
- A soft towel
Fix a routine to brush and clean your dentures at least once a day. Brushing them twice- every morning and before retiring to bed works even better. However, it is advisable that you don’t use toothpaste while brushing and cleaning your dentures.
Multiple mainstream toothpaste brands that are available in the market might contain ingredients that can prove to be too harsh and abrasive for your complete or partial dentures. Toothpaste in this category can eventually damage the surface of the dentures, leading to tiny cracks and scratches.
It is advisable that you brush your dentures with a gentle and soft-bristled toothbrush made especially for dentures. These toothbrushes are designed to prevent scratches and cracks on the surface of your dentures.
Brushing is important, however, only brushing doesn’t suffice to clean dentures alone. To maintain your dentures for a longer term, you are required to clean them thoroughly every night after taking them out.
Cleaning Instructions
Step 1.
Place a soft and clean towel on the counter before taking your dentures out. If you happen to drop your dentures accidentally, the towel with provide the necessary cushioning and save it from any damage.
Step 2.
Take the dentures out of your mouth and rinse to wash them with warm water.
Step 3.
Use a soft-bristled toothbrush to gently brush your dentures and remove the bacteria, plaque, and food particles from them. Clean all the surface areas of the denture. You can also choose to use a denture cleanser or mild soap and warm water. Brushing also loosens and gets rid of any denture adhesive. After the brushing is done, rinse it with warm water.
Step 4.
If you are retiring to your bed, soak the dentures in warm or lukewarm water. You can also use a denture-soaking solution to soak your dentures overnight. You don’t want your dentures to dry out. Dryness can lead dentures to lose their shape and become structurally more brittle. Rinse your dentures in the morning before putting them back on. It is recommended that you don’t soak your dentures in hot water. Heat can alter the shape and integrity of the material.
How Often Should You Clean Your Dentures?
Your dental health experts recommend that you thoroughly clean your dentures at least once every day. It’s even better if you could brush your dentures twice every day.
Brushing your dentures after you wake up in the morning and before wearing them back on. on the other hand, you should soak your dentures in a mild soap or a dental cleansing solution every night before retiring to your bed.
We have already mentioned that it is not ideal to use toothpaste to brush your dentures. However, you should brush your gums and tongue, with toothpaste at least two times every day. This helps you maintain the health conditions of your gum and prevents bad breath.
If you happen to have partial dentures, it is important that you don’t forget to brush and floss your remaining natural teeth at least twice every day.
Rinsing and cleaning your mouth with mouthwash also promote and contribute to the maintenance of oral health conditions. You might take off your dentures before using the mouthwash, or you can also choose to use mouthwash that has been specifically designed for denture wearers.
What Are the Best Ways to Maintain Your Dentures?
Dentures can last up to 7-10 years on average when they are maintained or taken care of properly and regularly.
Maintenance Tips
To prevent and control the build-up of food particles and debris, take off your dentures and rinse them with warm or lukewarm water after finishing your meals.
Dentures are structurally fragile and can break easily. You are required to handle them with care and take all the time you need to clean your dentures. It is important that you always remove and clean your dentures over a sink or bowl of water or over a clean and folded towel.
Some of the chemicals used in the making of toothpaste are too harsh for dentures. Don’t apply toothpaste or teeth whitening products to your dentures. Toothpaste with harsh and possibly abrasive chemicals, or dental whitening products can also change the color of the dentures.
Never sleep in your dentures- it is riskier than you can ever imagine.
It is crucial to soak your dentures in warm or cool water overnight, before going to bed. Hot water can lead to the deformation of dentures because of their temperature.
If your dentures happen to break, please get an appointment with your dentist. The broken dentures are not for you to fix. This is possibly going to do more harm than good, for the dentures.
If you are using denture adhesive, follow the instruction provided by the manufacturer properly and use only as much as has been advised. Remember to remove the adhesive from the dentures every night gently with a soft-bristled brush, mild soap, and water.
When To Call Your Dentist?
Schedule regular appointments with your dentist, at least twice every year or once every six months. If you are wearing dentures, schedule frequent appointments with your dentist as recommended by them. Also, get in touch with your dentist if you happen to have any concerns or queries about your dentures.
Make An Appointment If Your Dentures:
- Feel uncomfortable
- Slip or no longer fit properly
- Make noise when you talk or eat
- Appear visibly worn or broken
You Should Also Contact Your Dentist If You Develop:
- Mouth sores
- Bleeding gums
- Bad breath
If you happen to notice the signs and symptoms of a developing mouth sore, this is a cue for you to realize that your dentures no longer fit you properly and you have to see your dentist.
Takeaway
Dentures enable you to fix and enhance your smile and build your self-confidence. However, they will only keep doing so as long as you take proper care of your artificial dentures. Consistent and thorough cleaning not only extends the usability of the dentures but also helps you maintain your oral health and hygiene. It is on you to ensure that you soak your dentures every night in the right kind of solutions, and get in touch with your dental health expert in case of any complications.
 18 Apr 2023
18 Apr 2023 What Is a Dentoalveolar Infection?
Healthy teeth don’t hurt and cause a cranky child. If your child has been complaining of toothache or sensitivity, chances are that they might be suffering from dental decay, cavity, or a dentialveolar (relating to the teeth) infection. A dentoalveolar infection primarily affects your child’s teeth or mouth.
Here is a list of things that you need to know about dentoalveolar infections:
A dentoalveolar infection starts taking shape when bacteria penetrate the tooth through a cavity or fracture on the surface of the tooth.
An infection might also be a result of an impacted tooth, which is a tooth that could not sprout out of the gums for some reason.
If your child happens to be struggling with a toothache, tooth sensitivity to hot or cold food and beverages, or mouth swelling, you should bring that to the attention of your dentist.
A dentoalveolar infection is usually very easy to get rid of if diagnosed at an early stage. However, if left untreated, the infection can spread to other areas of the body and may result in a life-threatening situation.
This infection can be easily taken care of with antibiotics. In serious circumstances or instances of recurrence, that affected tooth/teeth might have to be surgically extracted.
Will It Go Away on Its Own?
There is no way that a dentoalveolar infection will go away on its own. If your child is struggling with the correlated symptoms, he/she will possibly need medical attention. In most cases concerning dentoalveolar infections, the primary effort is put behind getting rid of the infection without having to uproot the teeth. If that doesn’t work, they will have to be surgically extracted from your child’s mouth. Antibiotics are usually prescribed at the same time to heal the infection at the earliest.
How Serious Is It?
If diagnosed at an early stage, the dentoalveolar infection can be easily treated with the help of antibiotics or tooth extraction. If left unattended, however, the infection might spread to the other parts of your child’s mouth and even sneak into the bloodstream, leading to a serious condition called “sepsis”.
Approaches To Treating Dentoalveolar Infections
Your child’s specific treatment depends completely upon the symptoms and condition that he or she exhibits. Treatment can include everything from a simple prescription for antibiotics to the extraction of an infected tooth. The dental health expert is usually required to assess your child’s unique situation to curate and develop a treatment plan.
Symptoms & Causes of Dentoalveolar Infections
What Causes a Dentoalveolar Infection?
The infection takes shape when the bacteria penetrate the surface of the tooth through an unattended cavity or a chip in the enamel. It might also happen when a particle of food gets stuck in the soft tissue of the surrounding tooth.
What are the symptoms of a dentoalveolar infection?
If your child happens to exhibit any of the following symptoms, it is advisable that you take her or him to your dental health expert or pediatrician:
- toothache
- fever
- cheek swelling
- tooth sensitivity to hot, cold, or pressure
- swollen lymph nodes
- redness or swelling of the gums next to a tooth
If your child happens to have an abscess that ruptures, bad-tasting fluid or pus might fill his or her mouth. Even after the abscess has ruptured and the pain goes away, the source of the infection still needs to be medically treated.
Diagnosis & Treatments of Dentoalveolar Infections
How Do We Diagnose Dentoalveolar Infections?
The first step towards treating the dentoalveolar infection is forming a complete, specific, and accurate diagnosis of your child.
When you take your child in for an assessment, the dental health expert will thoroughly examine the affected tooth and the surrounding vicinity to look for swelling and other signs of infection.
X-rays help identify the abscess or impacted tooth.
A blood test might be necessary to look for signs of infection and its severity.
How do we treat dentoalveolar infections?
As mentioned, the treatment of your child depends completely on the cause of the infection and the pace at which it is progressing or spreading.
Infection Caused by Cavity or Fracture in The Tooth
The first step towards treating a dentoalveolar infection is to drain the infection. This might often be taken care of with the help of a root canal- a surgical procedure that is used to remove an infected nerve end from inside the tooth.
However, a root canal doesn’t always successfully save the affected tooth; and the infected tooth will have to be extracted.
After the infection has been drained out or the tooth has been taken out, the dentist is most likely to prescribe antibiotics to make sure that the infection-causing bacteria remains contained and doesn’t spread any further in your child’s mouth.
If the severity of the infection in your child’s mouth is on the higher end of the scale or is caused by an impacted tooth, she or he might have to stay in the hospital for a day or two to receive Intravenous antibiotics.
Impacted teeth might partially be hidden under the gum tissue. The food particle, upon entering the gap between the tooth and the gum tissue, an infection starts to take shape.
Antibiotics are prescribed to deal with the infection, but the infected tooth ultimately has to be extracted. The dentist will cut open an incision in the gum covering the impacted tooth, remove a tiny part of the bone, and extract the tooth. Sutures or stitches will be put to hold the gum together after the successful removal of the tooth.
How Can We Prevent Future Infections?
The best and easiest way to prevent any dentoalveolar infection is to make sure that your child maintains a good dental health and oral hygiene regimen. If you know that your child possibly has an impacted tooth, try bringing it to the attention of your dentist or an orthodontist to avoid any future hullabaloo
Preventing Tooth Decay and Cavities Involves Five Simple Steps:
Brush your child’s teeth and clean their tongue twice a day with a fluoride-based toothpaste, or monitor them while they do it on their own.
Flossing your child’s teeth is necessary on a daily basis, only after the age of 2.
You have to ensure that your child eats a well-balanced diet and refrains from consuming sugary snacks.
Consult your child’s physician or dentist about any supplemental use of fluoride and/or dental sealants.
Schedule dental cleaning sessions for your child’s teeth at least twice a year or every 6 months.
What Else Can We Do at Home?
The American Academy of Paediatric Dentistry recommends the following set of guidelines to ensure your child maintains a correct diet to have a healthy body and teeth:
- Ask your child’s dentist to help you evaluate your child’s diet.
- Don’t routinely stock your pantry with sugary or starchy snacks.
- Buy fun foods only for special occasions.
- Limit the number of sugary and starchy snacks and replace them with nutritious alternatives.
- Provide a balanced diet, and save foods with sugar or starch only for mealtimes.
- Don’t make it a habit for your child to go to bed with a bottle of milk, formula, or juice.
- If your child chews gum or sips soda, choose the ones without sugar.
What Is the Long-Term Outlook for Dentoalveolar Infections?
Maximum cases of dentoalveolar infections are taken care of with the help of antibiotics and cleaning out or the extraction of the infected tooth or teeth. However, the infection goes out of hand, might get slightly tricky to treat, and might need surgery or hospitalization. Rush your child to the dentist, orthodontist, or at least a pediatrician as soon as you notice the symptoms of an infection.
 18 Apr 2023
18 Apr 2023 DENTAL TRAUMA AND HOW TO DEAL WITH IT LIKE A PRO
What Is a Dental Injury?
A dental injury is primarily an injury to the mouth. It can lead to the following:
- Lost or displaced teeth
- Broken teeth
- Damaged gums
if you happen to have lost a tooth and still have the lost tooth in your possession, chances are that it can be saved. You should rush to a dentist or the hospital within half an hour of the incident. It might still be possible to save the tooth even after 3 hours of the injury.
What Symptoms Relate to A Dental Injury?
An injury to your mouth is likely to cause swelling, or worse even bleeding. If the blood flow is heavy, you must seek quick and urgent medical attention considering there are chances that your airway could get blocked or jammed.
Oftentimes, the damage or the injury to your mouth might not be completely visible. If there is a case of a cracked tooth, or a chipped tooth loose tooth after an unforeseen incident, it is important that you see a dentist almost immediately. This will save you a lot of future inconveniences, effort, and long-term damage.
The other signs and symptoms of a dental injury include toothache, and swelling of the gums.
What Causes a Dental Injury?
The most well-known and frequent causes of dental injuries are:
- Falling over
- Being hit in the face
- Having an accident while playing a sport
- Eating something hard
When Should I See My Doctor?
- It is always wise to call an ambulance or go straight to the emergency room if you see:
- The person is having trouble breathing
- There is a lot of blood going down the throat
- The mouth or tongue is very swollen
- if the injured person is breathing normally and the mouth is not bleeding too heavily, try to use a sterile dressing gauge or a clean towel to apply firm yet gentle pressure on the bleeding area. Then rush to the emergency room at the earliest.
- If your child or you seem to develop or experience the symptoms listed below, bring it to the attention of your doctor:
- Any difficulty talking or swallowing
- Swollen lymph glands in the neck
- A fever (a temperature over 38⁰c)
- If your child or you happen to experience a painful tooth, try fixing an appointment with your dentist as soon as possible.
Dental Injury First Aid
Lost Or Displaced Teeth
If your child happens to lose their first tooth or baby tooth, it is not wise to try to put it back in. Instead, rinse their mouth with salt water and apply a cold compress if there is mouth swelling, consult your pharmacies or your doctor about painkillers or pain relief medicines suitable for children. Please understand that this is not applicable to teething babies.
If an adult person has lost their tooth, try to restore it. The next logical step would be to call the dentist immediately and ask for an immediate appointment, ideally within the first 30 minutes of the accident.
Handle the detached tooth with absolute caution- it is advisable to hold it by the brown. This is the white visible part of the tooth that is there. Strictly avoid touching the root. Don’t rinse the detached tooth or try scrubbing it. If the tooth has dirt on it, rinse or soak it in milk. If you don’t happen to have milk at your disposal, use saliva or a sterile saline solution that is easily available in the pharmacies.
If there is a possibility where you might be able to push the tooth back into the socket it came from, do it until you hear a click or feel like the detached tooth is on the same level as the other teeth. Then bite down very gently on a sterilized cloth while making an immediate visit to the dentist’s office for further check-up and treatment.
Unfortunately, if you cannot push the teeth back in the socket, place or soak it in a saline solution or a glass of milk, immediately to keep it alive. Soaking or placing it in water is not exactly wise because it might damage the tiny delicate cells of the detached tooth.
If you don’t have milk or saline solution at your immediate disposal, place the detached tooth cautiously in your mouth- between your gum and cheek and then rush to the dental health expert. Try to not make it harder than it already is by swallowing the detached teeth by mistake.
You can also try to make use of plastic wrap or a zip-lock pouch to protect the detached tooth. Spit a little saliva into the plastic wrap or the zip-lock bag before sealing it in. A piece of cloth or tissue paper is never a good choice to transport a detached tooth to the dentist’s office.
Broken Teeth:
If parts or portions of the tooth have broken or chipped off, these tiny parts too should be soaked in milk or a sterile solution to keep them alive and then carried to the dentist’s office.
Swelling and Pain:
If there is swelling, try holding a cold compress against the swollen side of the face to ease the pain and reduce the swelling. cover or wrap the icepack with a clean cloth before placing it against your face.
How Is a Dental Injury Diagnosed?
The doctor, dentist or orthodontist will quickly asses the condition and get an X-ray. They are also likely to ask you about your pain and inquire about your dental history.
How Is a Dental Injury Treated?
The treatment plan will completely be pendent on the type of injury, dental history, and overall health condition.
If the injury also concerns the pulp of your tooth, chances are that you might need a root canal procedure.
If the injured tooth is only hanging by a thread or is completely detached or dislocated, your dentist or the orthodontist will first need to stabilize it and give it some time until your mouth heals. The medical expert will possibly do it by making use of a split or bonding it to the adjacent tooth.
A cracked or broken tooth might require a crown to save itself. These crowns are usually made of porcelain or metal. As we have already mentioned, an additional crown strengthens the integrity of the tooth and keeps it stable.
If your detached tooth cannot be saved, the chances are that your dentist or orthodontist will discuss the alternative options with you. Some extremely severe dental cases often require surgical assistance.
Can A Dental Injury Be Prevented?
A few actions and activities are comparatively more dangerous and accident-prone than others when it comes to causing dental injuries. Prevention is always better than cure, which is exactly why it is wise to wear a well-fitted mouthguard- that could possibly be personalized by your orthodontist to protect your teeth while indulging in activities like:
- Off-road bike riding
- Skateboarding
- Rock climbing
- White-water rafting
- Trampolining
- Boxing
- Football — soccer, rugby, league,
- Basketball
- Squash
- Hockey
- Old , damaged, or worn-out mouthguards require replacement for the sake of your safety.
- Consult your dentist and seek his advice about oral protection tips for your child and yourself.
- Complications Of a Dental Injury
A minor or severe dental injury is often followed by the risk of getting an oral infection. You can easily prevent this by maintaining good oral health and dental hygiene regimen and following the instructions given by your dentist.
It is very important that you pay adequate attention to a dental injury and get it fixed. If you don’t, the chances are that your mouth might develop a long-term ailment having a detrimental effect on your overall health. Dental injuries are bound to make it harder for you to talk, chew and swallow your food. This will have an impact on your nutrition and general health conditions.
ORAL HERPES OR HERPES SIMPLEX VIRUS
Overview
Herpes, also known as the Herpes simplex virus (HSV), is a common infection that is known to cause painful blisters and ulcers. It is communicable in nature and spreads by skin-to-skin contact. It is treatable though, though, cannot be completely cured.
There are two types of herpes simplex virus.
Type 1 (HSV-1) gets usually communicated by oral contact and is known to cause infections around the mouth (oral herpes or cold sores). It can also lead to genital herpes. Adults are usually infected with HSV-1.
Type 2 (HSV-2) spreads by sexual contact and causes genital herpes.
The majority of people don’t even have no symptoms or only mild symptoms. The infection can also cause painful blisters that might also recur over time. Medicines can only cure the symptoms but won’t be able to cure the infection.
The symptoms of both genital and oral herpes that recur over time tend to be very inconvenient and distressing. Genital herpes has an associated social stigma and has an impact on sexual relationships. With time, however, the maximum number of people struggling with herpes get used to living with the infection and try to live a decent life.
Symptoms
The majority of people don’t even have no symptoms or only mild symptoms. People often are not even aware that they are carrying the infection within them and might pass the virus along to others without even knowing it.
Painful, recurring blisters or ulcers are some of the recurring symptoms of herpes. Symptoms like fever, body aches, and swollen lymph nodes become visible when newer infections occur.
The symptoms might usually be different during the outbreak of the first episode of the infection as compared to the recurrent episode. If you happen to notice an occurrence of the symptoms, it usually does with tingling, itching, or a burning sensation where the sore is going to appear.
The symptoms of common oral herpes include blisters (cold sores) or open sores (ulcers) in or around the mouth or lips. On the other hand, the symptoms of common genital herpes includebumps, blisters, or open sores (ulcers) around the genitals or anus. These sores and blisters are usually painful in nature and also might break open, ooze, and then crust over.
During the initial days of the infection, people might come across:
- Fever
- Body aches
- Sore throat (oral herpes)
- Headache
- Swollen lymph nodes near the infection.
People can have repeated outbreaks over time (‘recurrences’). These are usually shorter and less severe than the first outbreak.
Treatment
Medicines are sometimes used to treat first or recurrent scenarios of herpes. They can help the longevity and severity of the occurrence of the symptoms, however, cannot be completely cured.
The treatment for the recurrent scenarios is getting an increased efficacy when started within 48 hours of the symptoms first beginning to appear.
Medicines used for antiviral purposed are usually prescribed. These medicines include acyclovir, famciclovir, and valacyclovir.
Consumption of lower doses daily of one of these medicines can also reduce the chances of the frequency of occurrence of the outbreaks.
Medical attention and treatment of the people who struggle with very painful and frequent recurrent scenarios or who wish to reduce the threat or risk of transmitting it to somebody else.
Painkillers and medicines are being used to seek relief from pain and painful sores including drugs like include paracetamol (acetaminophen), naproxen, or ibuprofen. There are also medicines that can be applied to numb the affected area including benzocaine and lidocaine
Herpes simplex virus resides inside the nerve cell and switches between being inactive and active.
Certain specific triggers that can activate the virus include:
- Sun exposure
- Menstrual period
- Injury
- Emotional stress
- Surgery.
Some people struggle with a special condition where herpes is activated by sunlight. Should that happen, try limiting your exposure to the sun and wearing sunscreen every time you have to go out to lower the probability of recurrences.
To reduce the symptoms of oral herpes, people can be advised to:
- Drink cold drinks or suck on popsicles
- Use over-the-counter pain medicines.
- For genital herpes, people can be advised to:
- Sit in a warm bath for 20 minutes (without soap)
- Wear loose-fitting clothes
- Use over-the-counter pain medicines.
There are ways to lower the risk of spreading herpes including:
Talk to your partner about having herpes
Don’t have sex if you have symptoms and always wear a condom (even when no sores)
Don’t share items that touched saliva (oral herpes).
Talk to your healthcare provider if you are pregnant, because there is a risk of passing herpes to your baby.
Scope Of the Problem
In the latest available data in 2016, around 3.7 billion people below the age of 50, or about 67% of the population worldwide, had HSV-1 infection (both oral and genital). In most cases of HSV-1, the chances are the infection has been acquired during childhood.
Genital Herpes
Genital herpes, triggered by HSV-2 affects an average population of 491 million or 13% of the people around the age between 15-49 years globally. Women are twice as likely to be infected by HSV-2 because the sexual transmission is twice as efficient from men to women. The prevalence however increases with age, although the highest number of new infections is among adolescents.
Transmission
HSV-1 is primarily communicated when there is direct content with the virus in sores, saliva, or surfaces in or around the mouth. HSV-1 can also be transmitted to the genital area through oral-genital contact and lead to genital herpes. It can also be transmitted from oral or on the surfaces of the skin that appears normal. The greatest threat of transmission occurs when there is the presence of active sores. People who are already struggling with HSV-1 don’t have the chance of getting reinfection but are still under the threat of acquiring HSV-2.
The primary pathway for the transmission of HSV-2 is sex- through direct contact with genitals o anal surfaces, skin, sores, or body fluids of the person already struggling with the virus. The sneaky HSV-2 virus can also be transmitted when the skin looks normal and there are no visible or tangible symptoms.
Under the rarest of rare circumstances, herpes (HSV-1 AND HSV-2) might be transmitted from a mother to a child during the process of delivery, leading to neonatal herpes among the babies.
Possible Complications
HSV-2 and HIV Infection
There is a heightened risk of acquiring the HIV infection if you are already struggling with HSV-2, at least by three times. Furthermore, patients both struggling with HIV and HSV-2 infection have higher chances of spreading the HIV infection among others. HSV-2 infection is some of the most common infections in people struggling with HIV.
Severe Disease
Herpes is known to have more severe symptoms and more frequent recurrences among immunocompromised people, including those with advanced HIV infection. A rare complication of HSV-2 comprises meningoencephalitis (brain infection) and other associated disseminated infection. On the other hand, HSV-1 infection can also lead to severe complications including ailments like encephalitis (brain infection) or keratitis (eye infection).
Neonatal Herpes
Neonatal herpes can occur when the infant gets an exposure to the HSV virus during delivery. Neonatal herpes is rare and occurs in around 10 out of every 100000 births around the globe. However, it is a difficult condition that can leave a long-term neurological disability or even death. The threat of neonatal herpes is the highest when a mother acquires the HSV for the first time during the advanced stages of pregnancy.
Prevention
People who have symptoms of oral herpes should steer clear from any oral contact with others, including oral sex, and sharing objects that get exposed to the saliva of the infected person. Individuals exhibiting the signs and symptoms of genital herpes should stay away from any sexual activity while the symptoms are still tangible. Both streams – HSV-1 and HSV-2 are the most contagious kinds when there are visible sores but can also be communicated when there are no tangible or visible symptoms.
For people who are the sexually active, proactive and correct use of condoms is one of the best ways to prevent genital herpes and others STDs. However, condoms only reduce the risk and the HSV infection can still occur when there is contact with genital or anal areas that remain uncovered by the condom. Medical circumcision among males can provide a life-long partial defense mechanism against the HSV-2 virus and infection, as well as against HIV and human papillomavirus (HPV).
People with tangible symptoms indicative of genital herpes should also be recommended HIV testing.
Pregnant women with tangible signs and symptoms of genital herpes should also bring that to their health providers. Preventing the transmission of HSV-2 infection is significantly important for women in the advanced stages of pregnancy when the risk of neonatal herpes is the greatest.
